They had just enough staff to run a virtual team three days a week, but they moved forward with a 90-day pilot, tracking metrics that they had identified at the outset. Using both in-room cameras and a cart model, they wanted to connect bedside nurses with virtual nurses who could provide an extra set of eyes. The pilot went so well that CoxHealth extended it for a year before embarking on a phased rollout across the system.
Nurses’ input was integral to the process and helped to secure buy-in. “Our nurses came up with a lot of the plans, and they came up with the workflows,” Ellerbee says.
Changing Clinical Workflows for the Better
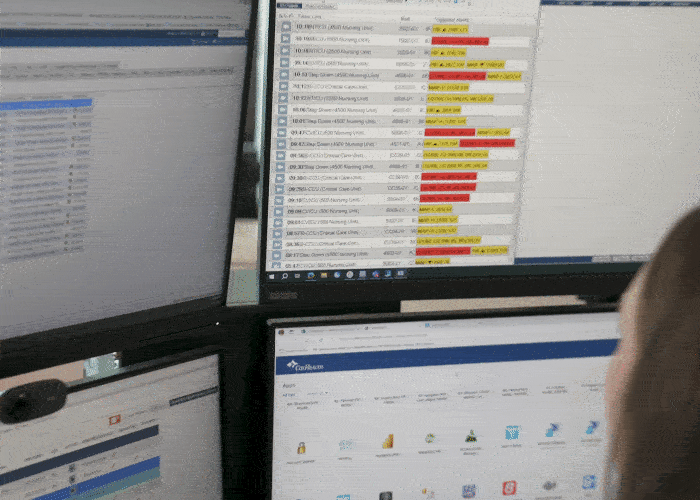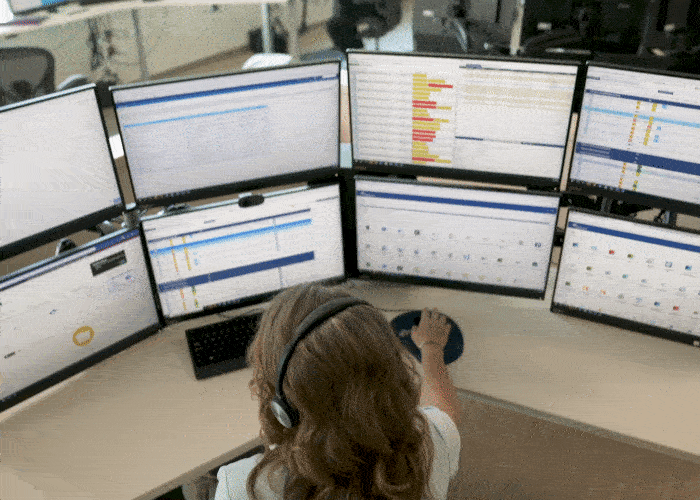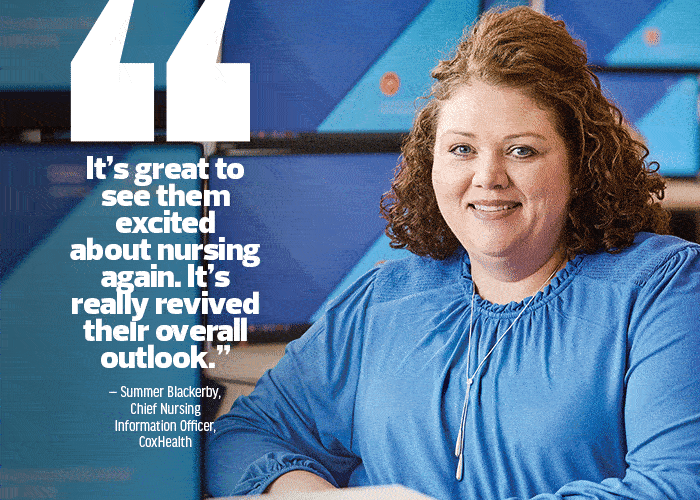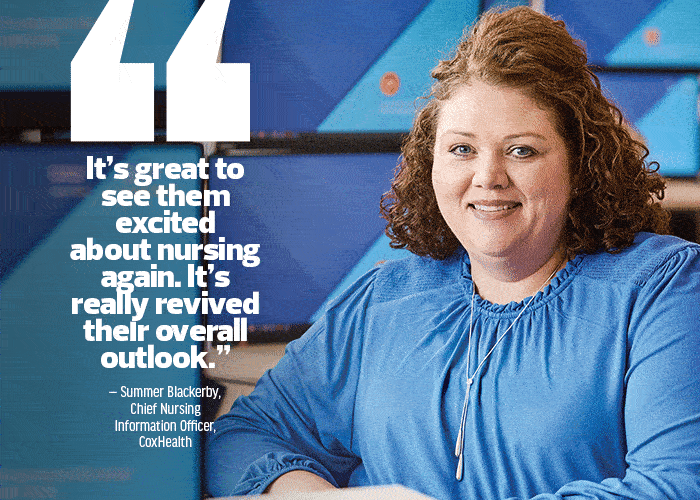
Today, a 5,000-square-foot virtual command center provides support for nearly 650 medical-surgical and intensive care unit (ICU) rooms. To join the virtual team, nurses must demonstrate excellent communication, clinical judgment and critical thinking skills. “It really is an elite place for them to be,” Ellerbee says.
IT solutions include Philips eCareManager enterprise telehealth software, Capsule Surveillance software, the Caregility platform and a centralized database of patient information.
LEARN MORE: Why integrating AI with virtual care transforms workflows and care delivery.
Electronic health record (EHR) system integration and AI predictive models in the Philips software pull in data that helps virtual nurses prioritize tasks. The command center provides early warnings so that nurses can attend to patient needs sooner. That has paid off with a reduction in falls, hospital-acquired infections and other issues.
Virtual care has been equally powerful for nurses, Blackerby says. “It’s great to see them excited about nursing again,” she says. “It’s really revived their overall outlook.”
Collaboration is the heart of the program. For example, if a medical-surgical nurse identifies a patient who needs extra attention, they can pull in an ICU virtual nurse, who may also tap an early intervention team on the floor. All work together to determine the best course of action.