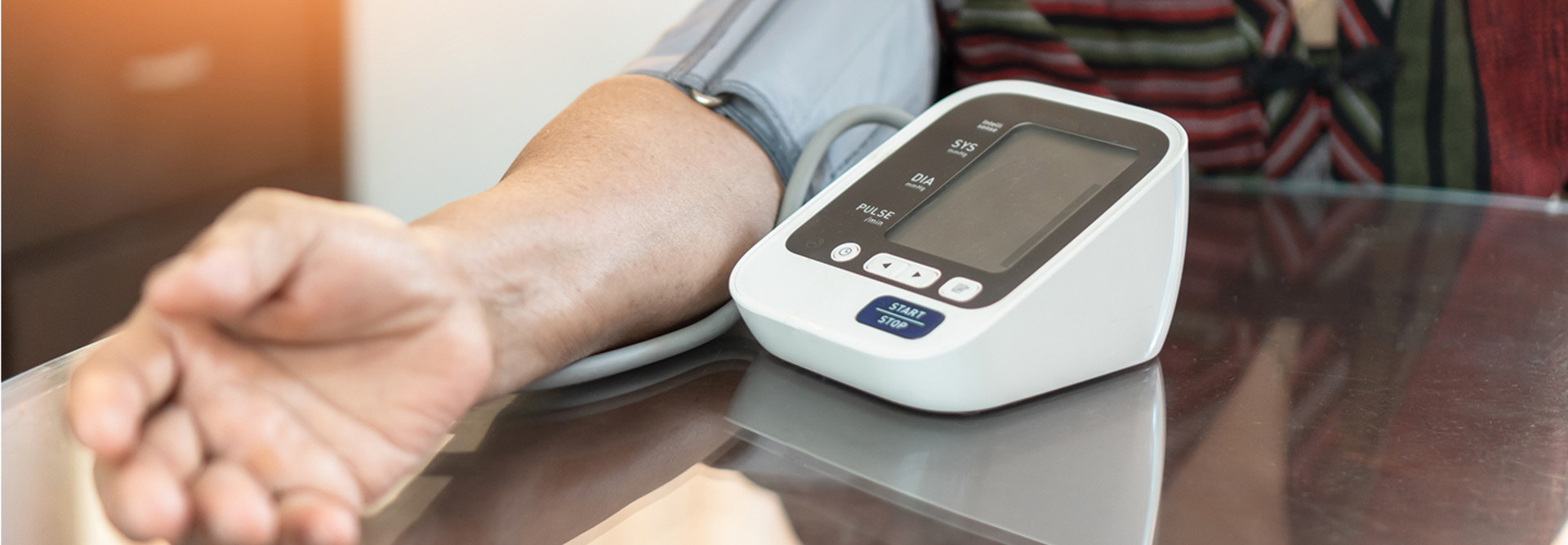
How Is RPM Data Collected and Analyzed?
RPM data can be collected in several ways. However, it is important for the data collection to be HIPAA compliant to protect patient privacy. Utilizing Bluetooth is the most popular data collection method. Typically, a healthcare provider will send the patient a kit with a glucometer, manometer or other Bluetooth-enabled device that connects to a smartphone or tablet to send patient data to the clinician. If the device has 4G capabilities, it can send data to the provider directly, without a wireless connection.
Having the proper application programming interface in place allows the data to be integrated directly into the electronic health record, making it easier for clinicians to keep track of a patient’s progress. The RPM-provided data can also be integrated into the billing cycle for reimbursement purposes.
Once data is collected, the clinician can then review and analyze it to ensure the correct procedures are being followed. Artificial intelligence with machine learning or deep learning is the future of RPM data analysis. These capabilities can provide additional preventive medicine by analyzing data trends, alerting clinicians so they can reach out to the patient to address any possible issues. AI also can improve cost and time efficiencies by analyzing data quickly so physicians can make faster diagnoses and treatment decisions. The more effective the algorithms, the more information that can be gathered.
MORE FROM HEALTHTECH: The benefits of remote patient monitoring are wide ranging.
Keys to Remote Patient Monitoring Program Success
The first steps to creating a successful RPM program are to get physicians and clinicians on board and ensure that the organization’s IT systems can support an RPM solution. Can the EHR integrate with the care management software? Who will handle that integration and support it in both the short and long term? These are questions that need to be considered prior to launching an RPM program.
Some patients will need consistent monitoring for chronic conditions such as congestive heart failure or COPD, while others will need less frequent or briefer monitoring. Healthcare providers need to categorize the patient and gather data appropriately.
It’s also important to evaluate RPM devices before choosing one for the program to ensure that it will be easy for patients to use. If patients are not comfortable using a device throughout the entire care cycle, the device could go unused or be used improperly, which may negatively impact the patient outcome or experience. The device or wearable should be ready to use once the patient receives the kit, and the healthcare organization needs to decide who will assist the patient if issues with the technology arise.
Healthcare is becoming more consumer-centric, and many patients now use monitoring devices such as the Fitbit or Apple Watch. Now that many patients are comfortable using telehealth, they are likely to expect — or demand — RPM services when appropriate. Health systems that do not provide RPM will likely fall behind the curve.
This article is part of HealthTech’s MonITor blog series. Please join the discussion on Twitter by using #WellnessIT.