Mobile Stroke Units Bring Emergency Care to a Patient’s Front Door
Speed is critical in caring for stroke patients. Every minute of delayed treatment translates into 2 million lost neurons, which dictates whether survivors will talk, walk or even survive, according to the National Stroke Association.
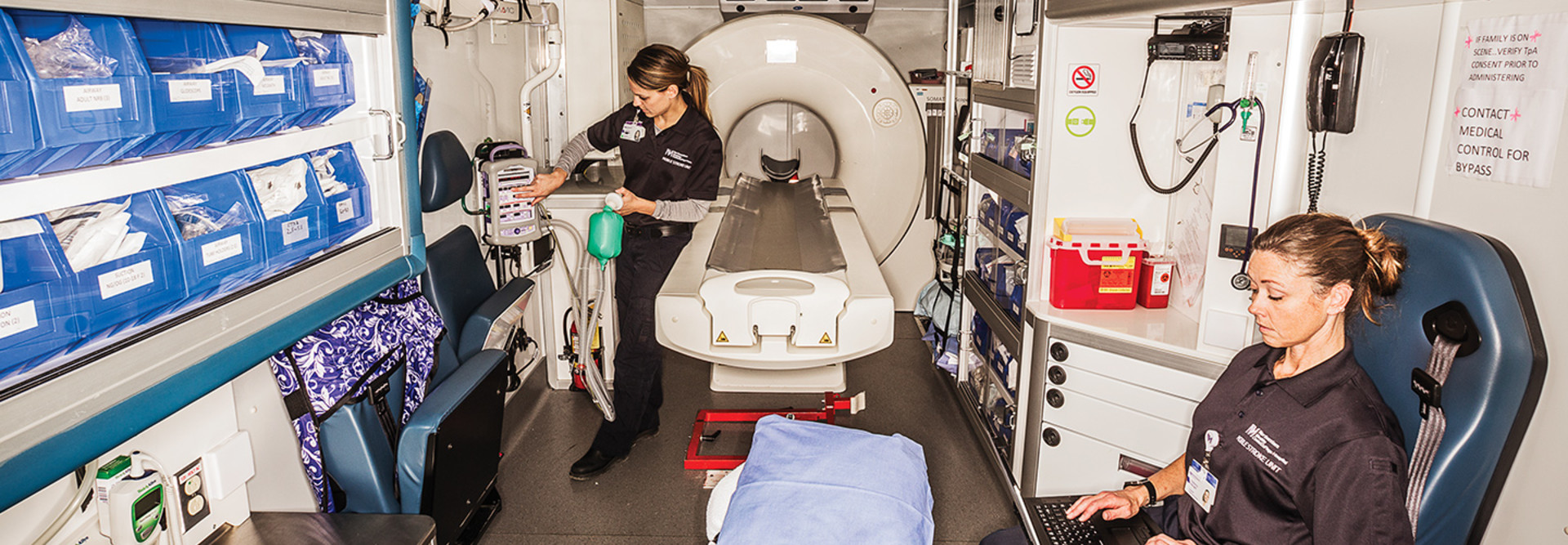
“Time is brain,” says Dr. Harish Shownkeen, medical director for the stroke and neurointerventional surgery programs at Northwestern Medicine Central DuPage Hospital (CDH). In January, the Winfield, Ill.-based organization deployed a mobile stroke unit — an ambulance outfitted with all of the medical equipment and technology necessary to triage, evaluate and care for stroke patients en route to the hospital.
In addition to an onboard CT scanner, the MSU is equipped with routers to transmit images to radiologists, as well as telemedicine and mobile tools for neurologists to consult remotely with patients, their families and the onboard stroke team.
“It’s basically a mobile emergency room,” says Dr. James Grotta, director of stroke research in the Clinical Innovation and Research Institute at the Houston-based Memorial Hermann-Texas Medical Center, which deployed the nation’s first MSU in 2014 in partnership with McGovern Medical School at UTHealth. “It keeps everything on four wheels and within arm’s reach.”
Today, roughly 20 facilities throughout the U.S. deploy the technology-enabled ambulances with a goal of delivering fast, reliable care in circumstances where every second counts.
SIGN UP: Get more news from the HealthTech newsletter in your inbox every two weeks
Overseas Inspiration Make U.S. Telestroke Units a Reality
With Shownkeen leading the way, CDH secured a $1 million grant to purchase its mobile stroke unit. The idea intrigued him after visiting Germany in 2014, where he saw one in action. Shownkeen watched as paramedics performed a CT scan on a patient in the vehicle and administered intravenous thrombolysis protocol.
“I could see the patient respond to the treatment right away,” he says. While Shownkeen initially wasn’t sure he could get the necessary buy-in to bring an MSU to Central DuPage, stakeholders surprised him with their optimism. “Everybody was convinced that this was a good way to give back to the community,” Shownkeen says. “It takes a village to get this thing done.”
Technology on board includes a Cisco Systems 829 Industrial Integrated Services Router, which Brian Weber, IS alignment program manager at CDH, calls the MSU’s “heart.” It also boasts redundant cellular accounts, so if the signal from the primary account drops, the router will automatically fail over to a secondary network.
The router transmits images from the CT workstation to the hospital, and also supports an HP Elite x2 1012 tablet, which runs a Motorola application that maps the most efficient route to the patient’s location. It supports a Panasonic Toughbook 54 Prime, which runs an emergency medical services reporting program and electronic health record software to register patients, order scans and document encounters.
Telemedicine Gets Stroke Patients Help in Minutes Versus Hours
Doctors can’t treat strokes until they identify their type. Ischemic strokes, caused by clots blocking blood from the brain, are treated with clot-busting drugs. Hemorrhagic strokes, on the other hand, form from ruptured blood vessels causing brain bleeds, so treatment involves reversal agents to stop bleeding.
Since the wrong treatment could exacerbate a stroke, doctors first must run CT scans to determine the cause. In traditional setups, paramedics evaluate stroke patients before transporting them to the hospital, where they then are triaged before undergoing CT scans and, finally, treatment.
With the MSU, they can begin treatment within minutes, instead of an hour or more. Joe Carrabba knows firsthand the importance of that rapid response. Following a stroke in June 2015, the Houston resident was one of the first patients to receive treatment in Memorial Hermann’s MSU.

The rig, which uses cloud-based medical imaging software, is staffed with a nurse, paramedic, CT technician and driver. Neurologists either ride in the MSU or use telemedicine technology to connect with the MSU team and patients remotely.
The unit is integrated with the fire department, so when 911 dispatchers identify potential stroke patients, they send it, as well as a standard ambulance. Together, they evaluate patients at the scene. If it’s a stroke case, the neurologist examines the patient or the MSU team consults with a neurologist via telemedicine, they run a CT scan and begin treatment prior to transporting the patient to the closest hospital. If it’s not a stroke, the standard ambulance transports the patient, making the MSU available for other calls.
Since August 2014, the MSU has operated on alternating weeks. For an ongoing trial, the health system tracks patients who received care in a standard ambulance versus those in the MSU to determine its effectiveness and value. Memorial Hermann is about halfway through the trial, consisting of 1,000 patients, but pilot data shows a statistical advantage among patients treated on the MSU, says Grotta.
In September 2016, the Patient-Centered Outcomes Research Institute awarded Memorial Hermann $6.8 million in funding to expand its research to hospitals in Denver and Memphis, Tenn., which also have launched MSU programs. Researchers are studying the outcomes of an additional 700 patients.
Carrabba, noting that his stroke occurred during an “on” week for the MSU, doesn’t take his good fortune for granted. “Everything lined up,” he says. “The first responders told my wife after the fact they didn’t think I would make it. I could have had a lot of neurological deficits, but I had none to speak of. I was out of the hospital in three days. I was like the miracle child of the wing.”
Account for Hurdles in Telestroke Adoption
CDH’s team has discovered challenges along the way, primarily related to the bandwidth demands of technology over cellular networks. To that end, Weber and his colleagues limited the technology inside the vehicle so nonessential devices wouldn’t consume all of the router’s bandwidth. “You really need to remember that this is an emergency situation,” he says. “The less distraction, the better.”
Each member of the MSU team has an iPhone 6s that utilizes a cellular plan separate from the router. The smartphones run a videostreaming app that provides the telemedicine connection between the MSU team and the CDH neurologist, as well as a backup program in case the Motorola application fails.
“One of the tenets that we have in this solution is to make sure we have at least one redundancy, if not two,” Weber says.

Simplicity is also important because of the limited space in the vehicle. Many MSUs have smaller mobile CT scanners, but CDH opted for a hospital-grade machine. While it requires a larger vehicle and more battery packs to support its increased power demands, the hospital wanted a more robust scanner capable of head, neck and chest scans.
The size can be a drawback, though, Shownkeen says. A narrow street might not accommodate the MSU, in which case a standard ambulance picks up the patient and meets the MSU at the nearest accessible location.
“It’s big. It’s bulky,” Shownkeen says of the rig. “It’s like a fire engine coming to your house.”
Still, he believes MSUs are a quantum leap in stroke treatment.
“This is the fastest, most efficient way of treating a stroke patient,” Shownkeen says. “It’s like taking the hospital to the patient.”