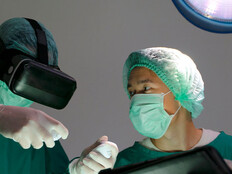
HEALTHTECH: How has the focus on the coronavirus pandemic affected the treatment of patients without COVID-19?
MCGILL: We still have a lot of patients who are fearful of coming into the healthcare system because they think they’re going to be exposed to COVID-19. We’ve tried to address those delays or gaps in care that have occurred, either due to fear from patients or limited availability of services. We also see that this could be magnified in some of the underserved populations, as we look at health inequities. So, we’ve tried to address that part of it as well, in a more proactive, individualized approach.
HEALTHTECH: Can you elaborate on what you’re seeing in underserved communities and how providers are responding?
MCGILL: This is not something new. We’ve always had concerns about the underserved communities, the patients who don’t have reliable housing, reliable technology connections, reliable transportation — all the social determinants of health. In addition to leveraging technology to improve our outreach, we’ve launched a universal social determinants of health screening: Every patient who comes in for an annual wellness visit or physical is screened for social determinant needs and then connected with resources.
I think now, with some of the increased awareness of social injustices that have been highlighted over the past year, people are more aware and realize that we need to address this. We need to actively intervene to address health inequities. We’re trying to leverage technology to identify patients at risk for health inequities. We’re increasing our resources to engage with those patients and redesigning our care models to address health inequities as well.
MORE FROM HEALTHTECH: See how artificial intelligence delivers healthcare efficiencies.
HEALTHTECH: What is the result of people not getting the care that they normally would?
MCGILL: Our concern is that we’re going to see cancers presenting at later or more severe stages. We’re going to see patients presenting with more advanced heart disease that could have been caught or prevented earlier or complications from uncontrolled diabetes.
We saw that very early in the pandemic, when patients were avoiding hospitals, so they were having heart attacks at home. Our concern is that will continue, with delays in getting routine care, screenings and preventative care; that we’ll see this wave, after COVID-19 quiets down, of patients coming in with what could have been preventable conditions. We don’t think we’ll see a higher number of cancer cases, but we’re fearful we’ll see higher rates of more advanced cancers.
HEALTHTECH: What are the implications from the perspective of healthcare providers?
MCGILL: At Community Health Network, we feel strongly that COVID-19, to some degree, is here to stay for the foreseeable future. Is that forever? Nobody knows. But at least in the now and near, the coronavirus is going to be around, so we need to learn how to deliver healthcare in a COVID-19 world. We can’t just shut down everything and manage the preventive care. We did that early in the pandemic, but now we’ve got to transition to a stage where we’re able to do both: take care of patients with and without COVID-19.
The impact on frontline clinicians, whether it’s doctors, advanced practice providers or nurses, is dealing with both in their day-to-day practice. That’s one of the things we’ve tried to focus on — how do you segment patients? Obviously, you don’t want to intermingle patients with COVID-19 and those without, but we’ve got to learn how to deal with both.
MORE FROM HEALTHTECH: How hospitals can leverage post-pandemic opportunities.
HEALTHTECH: How can the healthcare industry in general address these delays in care?
MCGILL:The first aspect is being aware that patients are fearful of interacting with the healthcare system. There’s also a financial aspect. People have lost their jobs or they’re not working as much, so that also is affecting care.
The second aspect is through education and creating systems to help patients feel comfortable. We’ve had marketing campaigns to communicate that, should you need to have an elective or emergency procedure, healthcare is safe. So, we need to educate providers and patients and develop the systems to connect patients with the resources they need.
Another factor is addressing the significant burnout among providers. One of our fears is that we’re going to see this mass exodus out of healthcare once the pandemic quiets down. While this is not a direct impact on people delaying care, not having enough providers will create more delays in care. We’ve tried to take a wellness approach and address some of the burnout because we’re fearful that providers will leave healthcare once the dust settles with COVID-19, that they’ll throw in the towel and say, “Look. I did it. I’m over the other side of the mountain, and I’m not doing that again.”
HEALTHTECH: How can technology help with these issues?
MCGILL: First and foremost, technology can help with identifying patients at risk for delays in care or patients that have actually had delays or gaps. Technology can also help in providing outreach. Jvion, the AI platform we use, allows for personalization of how patients want to be contacted, whether by text, email, phone or in person. So, technology can take some of the friction out of the healthcare system that existed before COVID-19 and that will exist afterward. We’re trying to leverage the technology to offload some of those activities from clinicians and make it a more frictionless experience for the patient.
HEALTHTECH: How is Community Health Network doing that?
MCGILL: We’re implementing Jvion to help with patient identification. We’ve had other enterprise partners help to automate and digitalize the outreach so that we’re not dependent on phone calls. We’ve implemented texting. We’ve expanded MyChart. We’ve automated some of the care coordination and patient outreach after a visit. We’ve done home monitoring after early discharges.