Innovative Hospitals Tap Automation to Streamline Patient Care
Automation might be one of those words everyone fears, as many believe it will eliminate jobs, but in the medical world automated processes play an important role in mitigating physician burnout and improving patient engagement.
And in many cases, hospitals across the country are already adopting automation to streamline workflows.
Stanford Children’s Health, located in Silicon Valley, and NYU Langone Health in New York, for example, are two hospitals that have integrated technology tools and applications to automate hospital operations and to improve communications and patient care.
Automation Makes the Difference at Kimmel Pavilion, Lucile Packard
At NYU Langone’s new Kimmel Pavilion, for example, the IT department has integrated the hospital’s electronic health record system with another internal healthcare workflow application. When a patient is discharged, the electronic health record automatically notifies the workflow app that the patient’s room needs to be cleaned, so it schedules the housekeeper staff to clean the room, says Ruth Harris, NYU Langone’s senior director of solution development, campus transformation.
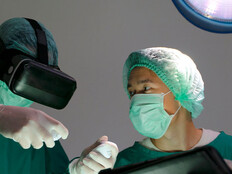
The IT staff at Lucile Packard Children’s Hospital Stanford in Palo Alto, Calif., meanwhile, is improving communications and the flow of information by integrating nurse central stations with patient monitors, the nurse call system and the medical staff’s iPhones, says Ilir Kullolli, director of clinical technology and biomedical engineering.
The hospital uses a mix of wired and wireless patient monitors that measure vital signs, such as heart rate and oxygen saturation level, and detects medical situations such as atrial fibrillation. The real-time patient information is sent to monitors located in nurse central stations at each unit.
From the central stations, each patient’s vital signs are recorded on his or her EHR, and any alarms or requests by the patient is sent to the staff’s iPhones, Kullolli says.
Using middleware software, the IT staff have programmed the system to direct alarms or patient requests to the appropriate doctors or nurses, based on the severity of the situation, says Alan Laver, the hospital’s IT application services manager.
For example, if a patient wants ice or wants to talk to a nurse, those requests are funneled to the iPhones of nursing staff who are assigned to the patient’s room. But if it’s a Code Blue emergency, everyone in the unit is immediately notified, he says.
The middleware software also integrates with the hospital’s real-time location system, so it knows when a nurse is in a patient’s room. If a patient alarm goes off, the system automatically knows the nurse is already in the room and has received the alert by the bedside, so it stops the nurse from receiving the same alert on the nurse’s iPhone, says Chee Yee Letterman, an IT project manager at Lucile Packard.
To learn more about how these innovative healthcare organizations are tapping technology to improve care, check out our feature "Hospitals Look to Innovation to Inspire Design."