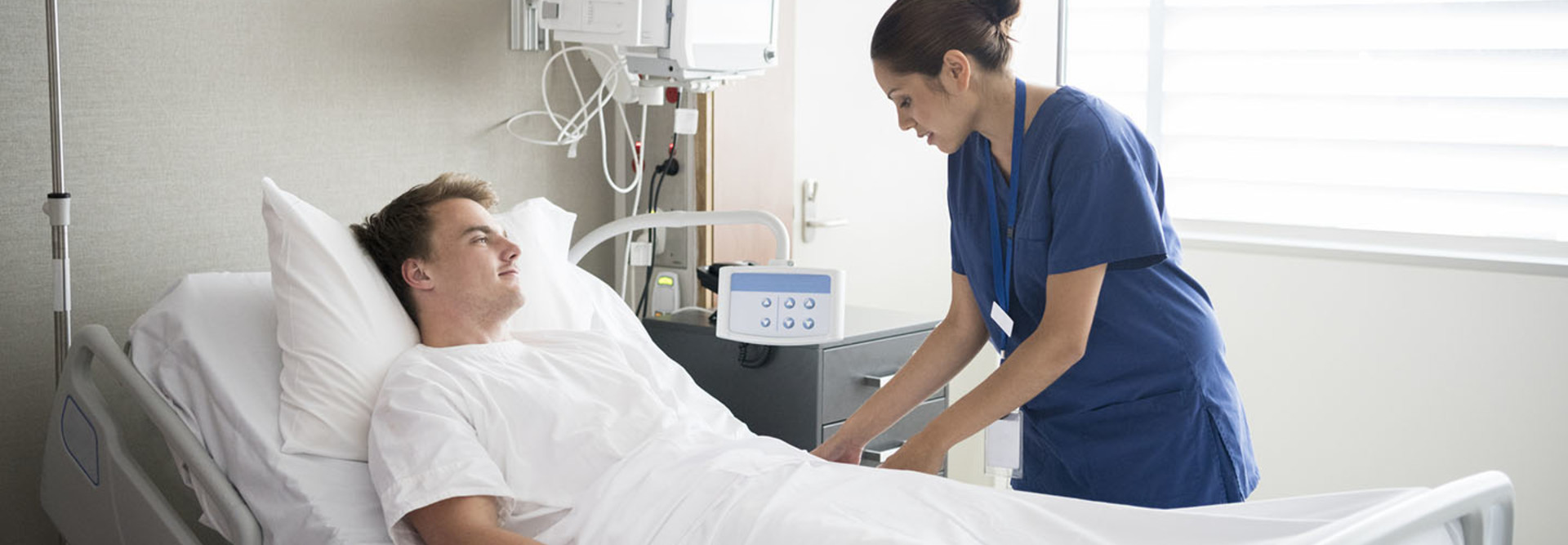
Parkland Health Embraces Mobility to Bridge Care Gaps Between Nurses and Patients
The busy nursing staff at Parkland Health & Hospital in Dallas needed a better way to communicate at the point of care. And when the hospital relocated from a 65-year-old building with an approximately 1 million-square-foot campus to an all-digital, 2.1 million-square-foot, 862-bed hospital, it gave them the opportunity they needed to do so.
“This was a massive transition — not so much apples to oranges, but more of an apples-to-watermelons type of change in scale and technology capabilities,” says Joe Longo, vice president of IT enterprise technologies at Parkland Health & Hospital System. “One of the main shifts was in the mobile-enabled space.”
Thanks to its one-foot-thick concrete walls and half-inch rebar, the previous hospital location didn’t have the best wireless connectivity.
“Our mobile communication infrastructure relies heavily on wireless connectivity, leveraging Voice over IP (VoIP). The old hospital environment posed many barriers to doing major advancements in the mobile space,” says Longo, noting that the old hospital required staff to rely on outdated pager technology as well as a lot of overhead paging and announcing, which could be disruptive to patients, families, visitors and staff.
Moreover, when Parkland moved into a space nearly twice the size of the old hospital, the nursing stations were naturally more spread out, which required the hospital to place nursing substations between every two inpatient rooms so the nurses would be closer to the patients.
“That proximity to the patient solved a lot of problems and right-sized our patient rooms to provide a superior healing environment, but it also created a more spread out environment. This created a new challenge for communication, in spite of solving many other problems,” says Longo.
Mobility Brings Patient Alerts Directly to the Caregiver
To remedy these new communication challenges, Parkland turned to new mobile capabilities. Specifically, to start pulling the communication in “tighter,” Parkland leveraged Zebra Technologies’ MC40 mobile computers and Workforce Connect app to provide the nursing staff with reliable VoIP. Alongside these new tools, the hospital also leveraged other apps on the WFC platform that enabled secure texting and allowed the staff to communicate with patients via text.
Parkland also leveraged alert and alarm aggregation apps to help find an available clinician to attend to a patient.
“If a biomedical device is alarming locally, we can send a secondary alarm message to the appropriate clinician, and if that clinician is unable to address the alert within a time period dictated by clinical leadership and patient safety, it will then roll over to the next person or persons, until someone addresses the alarm,” Longo explains.
Overall, the mobility program was able to solve many of the communication problems the nurses were having as well as make clinicians constantly available via secure phones. It also offered clinicians the ability to access emergency medical records and receive any alerts or notifications that might come along with the EMR access.
“Really, the paradigm shift is that we used to be local or logged in to a system, watching a screen, to receive these notifications. Now those alerts and notifications are pushed directly to the caregiver wherever they are in a very large organization,” says Longo. “It is incredibly valuable to give that connectivity to the caregiver in real time. Now, we also have bidirectional acceptance of, “Hey, I’ve got it.” And if that doesn’t happen in the appropriate time frame, it will roll over to another person who will respond to the patient need.”
Informatics Ownership Makes Mobility in Every Unit a Success
The rollout didn’t happen overnight, however, and there were several cultural and technical barriers to work through before the adoption was fully rolled out and accepted among nursing staff.
Many stakeholders were concerned that the IT infrastructure might not be able to meet the required specifications for a reliable wireless mobile experience.
“We wanted to ensure that we had thought out the foundation of the technology, considering the criticality of the communications was so high and, in many cases, directly linked to patient care, in which there is no room for error,” says Longo.
Moreover, to mitigate any hesitancy the nursing staff might have around using the new technology, the IT team implemented simulations and onsite training prior to the transition into the new facility.
“We held ‘Parkland Fridays’ which were dedicated to taking the staff across the street and letting them use the new devices and perform new workflows in the new physical space,” says Longo. “We set up a booth with the new technology devices and clinicians were allowed to play around with them and practice using the new applications. Allowing the staff to test the technology and gain a comfort level before actually using the technology in the real-time setting proved to be very beneficial.”
The most crucial aspect of the successful rollout, however, was the engagement and ownership that Parkland’s nursing and clinical informatics group had in the project.
“They were instrumental in getting out to different units,” says Longo, noting that it became evident that the needs of some units differed from adjacent units. For example, Longo says the neonatal intensive care unit, which has 96 individual ICU rooms over a very large space, has different needs for communications, alerts and alarms than those of a medicine unit.
“The heavy reliance on both nursing and clinical informatics teaming up with the clinical end users in their differing areas was incredibly effective and ensured we didn’t attempt a one-size-fits-all methodology,” says Longo. “They helped train, configure and adjust the system to accommodate the needs of every unique department while leveraging the technology to facilitate better patient care.